
Designing Effective Communications for your Community
On this page
The COVID-19 pandemic has exposed deep health inequities in the U.S. Vulnerable populations have been disproportionately impacted by higher rates of COVID-19 infection, hospitalization, and mortality. The White House has put equity at the center of the response to the pandemic and subsequent economic crisis. For the U.S. to reach herd immunity, we have to focus on communication surrounding vaccine hesitancy, mistrust in government, lack of access, and other equity issues facing underserved communities and vulnerable populations.
To date, a few guides focused on vaccine communication strategies exist; however, there is a need to augment these with approaches specific to vulnerable populations. This playbook also enables efficient and effective counter response to mis/disinformation in a fast-changing environment.
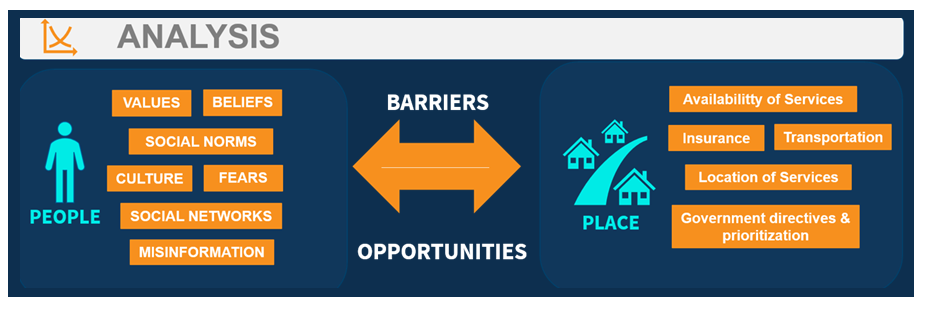
The Peoples and Places Framework provides an approach for combining communication and marketing principles for the purpose of achieving public health objectives. The playbook uses this framework for understanding vulnerable populations. It focuses on key factors of “people and “places” that influence both individual health behavior as well as the health of the larger community.
This playbook, the focus will focus on the key factors of People and Place for vulnerable populations, specifically at the community level. When conducting an analysis of a vulnerable population, it’s important to remember that “one size does not fit all.” A vulnerable population in one geographical area of the country will not be the same in all areas of the country. For example, Native American tribes will differ in attributes of people and place depending on the tribe. An analysis of each community must be conducted in order to design effective, customized health communication interventions.
Health literacy
Public health communication campaigns should always consider levels of health literacy early in the development process. Health literacy is the degree to which individuals can obtain, process, and understand basic health information needed to make appropriate health choices. Vulnerable populations such as older adults, minorities, those with limited English proficiency, and underserved communities are at risk for having lower health literacy rates.
There are ways to craft messages that resonate across all levels of health literacy.
- Use everyday words (example: vaccines are commonly called ‘shots’; instead of using ‘doses’ use the word ‘times’)
- Use short, concise sentences
- Use clear and direct calls to action (example: Get a COVID-19 vaccine to help save lives.)
- Make adequate use of white spice to break up text
- Use simple videos, photos, or graphics to convey the message
- Run your messages through the CDC’s Clear Communication Index. It can provide a health literacy ‘score’ for both short and long form communication, which allows you to adjust if needed. Link https://www.cdc.gov/ccindex/index.html
Social determinants of health
Conditions in the places where people live, learn, and work greatly affect health risks and outcomes. These are known as social determinants of health – and they are responsible for most of the health inequities and disparities seen globally and here in the U.S. Examples of social determinants include socioeconomic status, physical environment, employment, transportation, healthcare, and many more.
The COVID-19 pandemic further revealed how social determinants of health can perpetuate and exacerbate inequities and disparities in health outcomes. For example, a person’s employment in a restaurant or janitorial position put them at further risk of contracting the virus because they could not work from home and quarantine. These jobs tend to be lower-paying and hourly-waged, with few benefits. Vulnerable populations disproportionately work these jobs and were therefore disproportionately exposed to COVID-19. health disparities that are often rooted in social and economic disadvantages.
- Develop messaging that is at the appropriate health literacy level for the target population and is written in plain language.
- If using digital communications, ensure that the target audience has access to the content and is at the appropriate literacy level to understand the content provided
- Use communication channels and sources most used by the target audience to deliver health information.
- Identify solutions to overcome the specific socioeconomic barriers that may prevent a target audience from vaccine adoption.
- Use the native language of the target audience when develop health messaging.
- Design health messaging is culturally appropriate.
- Account for any cognitive, visual and auditory limitations/barriers that can impact the ability of the older adults to get vaccinated when designing the health messages
Acknowledge historical abuses/trauma in medical care and research
Understanding and acknowledging the reasons behind an individual or group’s skepticism about vaccines is critical to the design of COVID19 vaccine communication efforts. Historical discrimination, injustice, and unethical medical practices have disproportionately affected minority communities. These traumas remain deeply woven into collective memory. These communities are, understandably, deeply distrusting of government and healthcare systems in the U.S.
- Reaching historically underserved populations, such as Black and Indigenous Americans, requires transparency and trusted, in-community messengers.
- Information and discussions from in-group minority scientists and healthcare professionals who were a part of the COVID19 vaccines development may begin to chip away at the reluctance to get vaccinated.
- Personal stories from community members who received the vaccine (and why) are also recommended.
Choose the right messenger
Barriers: Lack of Trust in Health Information
Trust plays a major role in effective communication with a community. Oftentimes, health communication campaigns use government leaders as the spokesperson. For communities that are distrustful of the government, elected officials may not be the best choice to communicate health messages.
Opportunities:
Community Opinion Leaders
Choose leaders within the community, who have already established trusting relationships with its members such as faith leaders, community healthcare providers, and small business owners.
Frontline workers
Consider frontline workers, who interact with community members everyday and have developed trusted relationships, deliver the messages. They are in the places where community members most frequent such as health centers, churches, barbershops, beauty salons, community centers , senior centers, local pharmacies, bingo halls, and small community grocery stores. These can also be groups consisting of trusted lay community members who can share health information directly with their community. Because they are from the community, they understand local culture, beliefs, norms and values and can break through communication barriers such as language.
Gatekeepers
Identify who the gatekeepers are in the community. These respected community members control information that flows to the people that you want to reach.
[Example] The familial gatekeeper
In different cultures a particular family member such as the abuela in the Latino community decides what information and health services should be accessed by the rest of the family, and even, whether or not family members should get a COVID-19 vaccine. Health communication efforts can focus on educating them on the COVID-19 vaccine. Health campaigns can also leverage these familial gatekeepers to assist in the formative evaluation of health messaging and communication strategies.
Use communication vehicles that resonate with specific communities
Barriers: Preferences for Receiving Communication Messages
In all geographic areas, whether it be a county, city or town, there are diverse communities consisting of different race and ethnicities with their own cultural beliefs, values, social norms, and language. Not only is the right message important but also how that message is delivered.
Opportunities:
We have already discussed the importance of identifying the messenger. But of equal importance is understanding where a particular community goes for health information such as ethnic media, local news, online social networks, word of mouth, community newspapers, ethnic radio stations, information sheets, etc. Consider digital literacy levels before focusing on a predominantly online campaign.
THIS IS A CHECKLIST CALLOUT BOX
ethnic media, local news, online social networks, word of mouth, community newspapers, ethnic radio stations, information sheets in community’s primary language
Resources
- Clear Communication Index from CDC: allows communicators to run their campaigns/messages through a checklist to ensure they are written at appropriate levels of health literacy/numeracy. Available for both short and long form messages (link)






